Author: Magdent Editorial Team
Published on: 07 March, 2026
This case, performed by Prof. Alberto Monje, involved a patient diagnosed with peri-implantitis, presenting with advanced bone loss and bleeding on probing. The treatment followed a surgical regenerative protocol combining mechanical decontamination and biological stimulation using the Magdent Miniaturized Electromagnetic Device (MED).
The procedure included implantoplasty, thorough surface debridement and decontamination, and guided bone regeneration (GBR) with a particulate bone graft and collagen membrane to restore the lost peri-implant bone structure. Immediately after the regenerative procedure, the MED healing abutment was connected to the implant and left in place for three weeks, delivering continuous pulsed electromagnetic field (PEMF) stimulation to promote cellular activation, angiogenesis, and bone remodeling at the defect site.

Outcome:
This case highlights the effectiveness of the surgical peri-implantitis management protocol integrating PEMF technology, showing how the MED device can enhance bone regeneration and accelerate healing when combined with conventional regenerative techniques such as implantoplasty and GBR. The synergy between surgical decontamination and electromagnetic stimulation supports a predictable, biologically driven regeneration in peri-implant defects, offering a viable alternative to more invasive resection procedures.
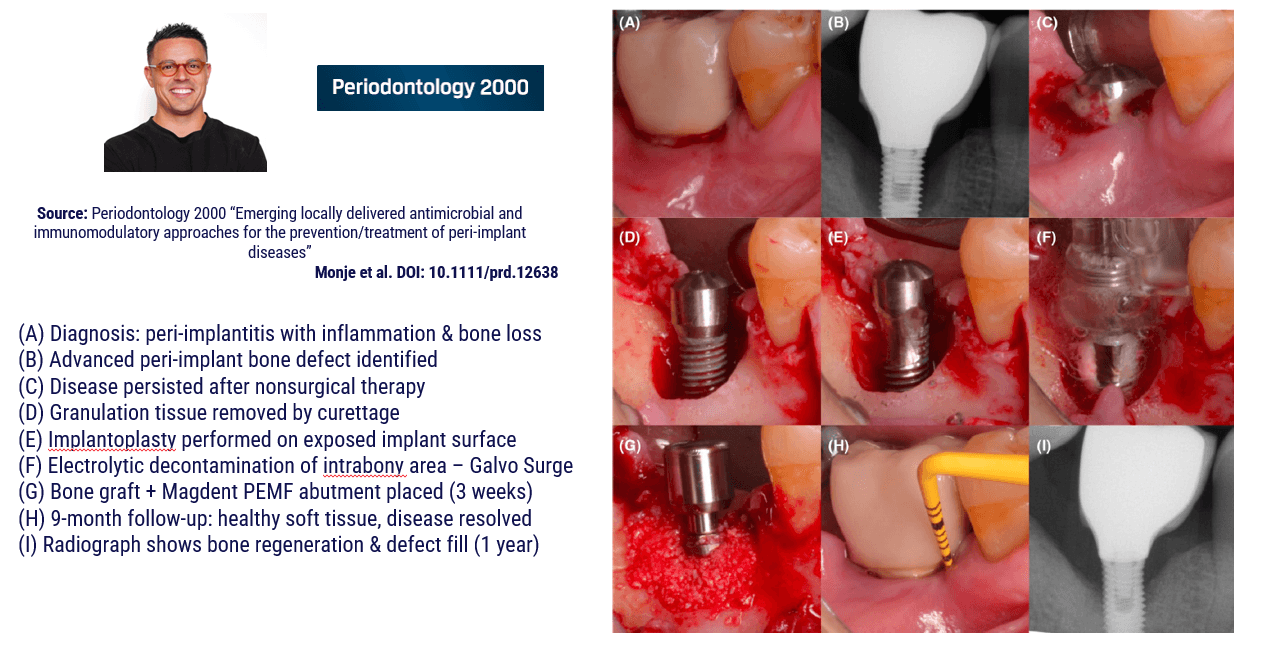
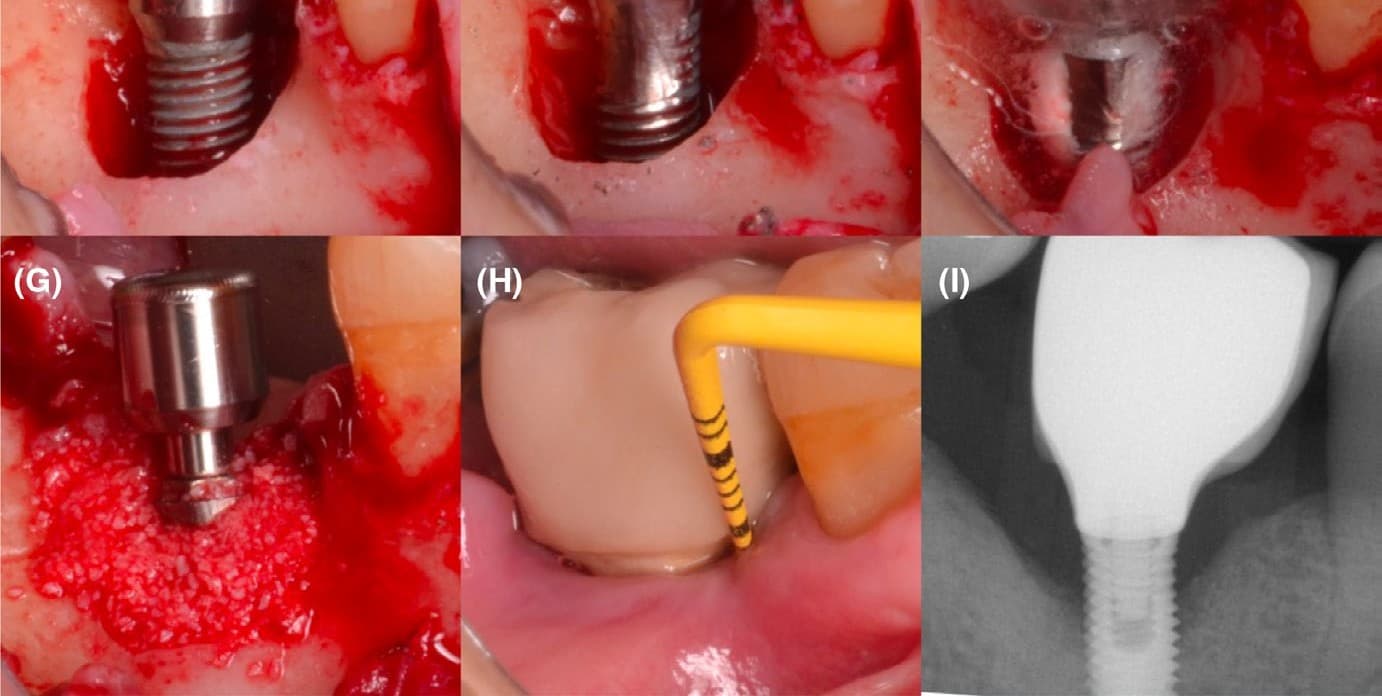
This clinical case, documented by Prof. Alberto Monje and published in Periodontology 2000 (“Emerging locally delivered antimicrobial and immunomodulatory approaches for the prevention/treatment of peri-implant diseases,” Monje et al., DOI: 10.1111/prd.12638), presents a surgically managed peri-implantitis defect with the integration of Magdent’s Miniaturized Electromagnetic Device (MED) as an adjunctive regenerative tool. The patient was diagnosed with peri-implantitis accompanied by inflammation and progressive bone loss (A–B). The disease had persisted despite prior nonsurgical therapy (C). During the surgical phase, granulation tissue was meticulously removed by curettage (D), and implantoplasty was performed on the exposed implant surface to smooth irregularities and reduce bacterial adhesion (E). Subsequent electrolytic decontamination of the intrabony area was performed using the GalvoSurge system (F), ensuring optimal surface disinfection prior to regeneration.
Following decontamination, a guided bone regeneration (GBR) procedure was performed using a particulate bone graft, after which the Magdent PEMF healing abutment was immediately connected to the implant (G). The MED device delivered pulsed electromagnetic field (PEMF) stimulation over a period of three weeks, enhancing cellular activity, vascularization, and bone remodeling during the early healing phase.
Outcome:
This case underscores the clinical efficacy of combining regenerative surgery, decontamination, and electromagnetic stimulation. The synergy between implantoplasty, electrolytic cleaning, and Magdent PEMF therapy demonstrates a predictable, minimally invasive, and biologically enhanced approach to peri-implantitis management, providing both functional and histological regeneration outcomes in previously compromised implant sites.
A patient presented with severe peri-implantitis, showing a probing depth of 6 mm and advanced bone loss. The implant was initially considered non-salvageable and scheduled for extraction, especially as an adjacent implant had previously been removed due to the same condition. The case represented a critical-stage peri-implant infection, typically associated with poor prognosis and progressive bone destruction.
Treatment Approach:
Instead of proceeding with implant removal, Dr. Eli Raviv implemented a regenerative, non-surgical treatment protocol using the Magdent MED healing abutment. The first MED device was placed for 30 consecutive days, delivering localized Pulsed Electromagnetic Field (PEMF) stimulation directly to the peri-implant site. After completion of the first cycle, a second MED was installed for an additional 30 days to extend the stimulation period and maximize regenerative outcomes. Throughout the treatment, no additional surgical intervention was performed.
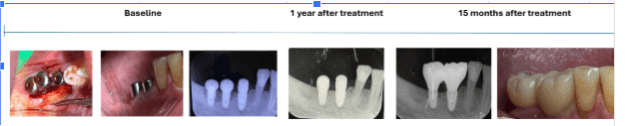

Outcome:
This case demonstrates the potential of MED-based PEMF therapy to reverse severe peri-implantitis in cases once deemed unsalvageable, providing a non-invasive, regenerative alternative that restores implant stability, bone integrity, and long-term peri-implant health.
A 71-year-old healthy patient with poor bone quality presented following failure of a previous implant. A new implant was placed using a MED healing abutment to enhance the healing environment and promote bone regeneration. Radiographic evaluation at insertion revealed low bone density around the implant site.
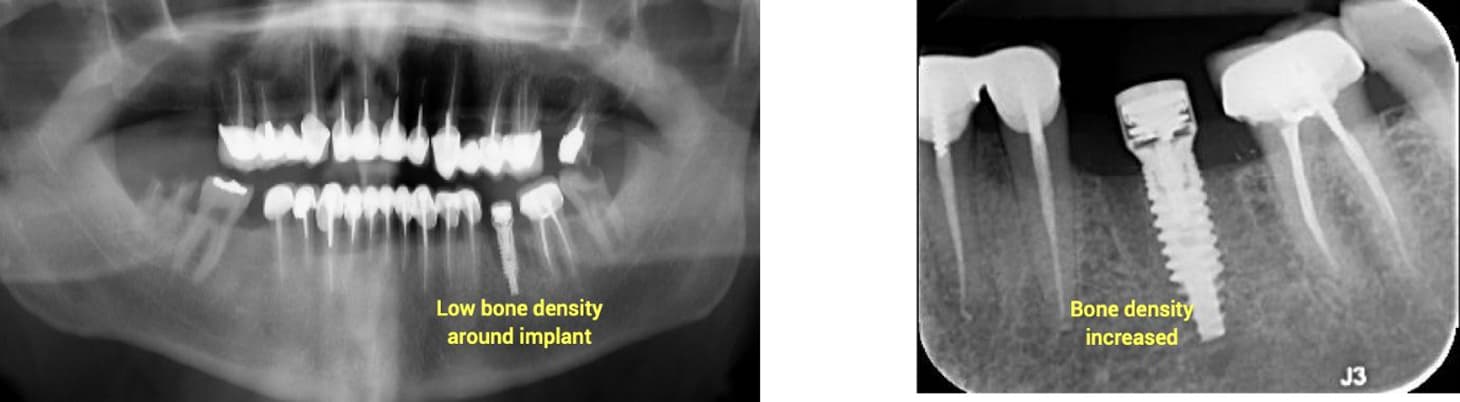

After 60 days, radiographs demonstrated a marked increase in bone density surrounding the implant, indicating successful osseointegration and restoration of bone volume. The improved peri-implant bone quality enabled a stable impression and subsequent prosthetic rehabilitation, confirming the effectiveness of the MED healing abutment in supporting bone regeneration and implant stability in compromised sites.
A 71-year-old healthy patient presented with a fractured implant, which required replacement. A new implant was placed and activated using a MED healing abutment to promote accelerated osseointegration and enhanced bone regeneration. The healing process progressed smoothly, with excellent tissue response and no complications observed.

After 60 days, radiographic and clinical evaluations confirmed complete osseointegration of the newly placed implant. The patient received a definitive crown, demonstrating strong implant stability, healthy peri-implant tissue, and optimal esthetic and functional results, validating the regenerative and acceleration benefits of the MED technology.
A 70-year-old heavy smoker presented with a fully edentulous mandible and clinically poor bone quality. Six implants were placed, each fitted with a MED healing abutment to enhance bone regeneration and support early osseointegration. Despite the compromised bone condition and smoking-related healing challenges, the patient demonstrated an excellent biological response throughout the recovery phase.
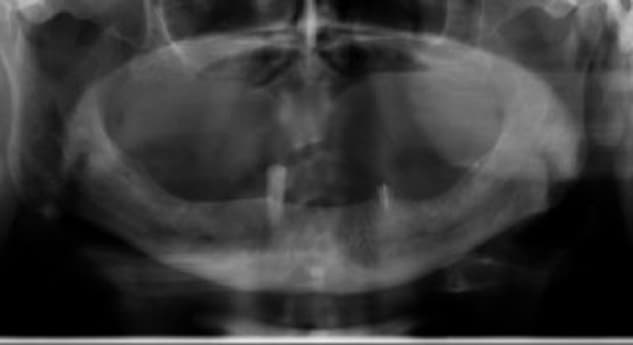
After only 45 days, radiographic assessment confirmed successful osseointegration across all six implants, allowing for full-arch prosthetic restoration. The patient received a stable mandibular bridge within a significantly shortened treatment period. The use of MED healing abutments contributed to rapid bone maturation, improved implant stability, and an accelerated rehabilitation process even in a high-risk, heavy-smoking patient.
A 55-year-old heavy smoker underwent a comprehensive maxillary rehabilitation procedure that included sinus lift and ridge preservation following tooth extraction. Three months post-extraction, implant placement was performed along with crestal sinus augmentation using MED healing abutments to enhance bone regeneration and accelerate osseointegration. Despite the patient’s smoking habit and compromised healing potential, bone regeneration progressed rapidly with excellent clinical and radiographic outcomes.


Within less than three months from implantation, the patient achieved complete osseointegration and received the final fixed restoration in the upper jaw. Radiographs demonstrated substantial bone regeneration around the implants and stable ridge contour, confirming the effectiveness of the MED healing abutments in promoting accelerated healing and predictable results even in challenging cases involving sinus lift and ridge preservation procedures.
A 73-year-old female patient with long-standing type II diabetes mellitus (average glucose level ≈ 200 mg/dL) presented with edentulism of the lower jaw and poor bone quality, classified as D4 bone - characterized by thin cortical plates and sparse trabecular bone. Seven implants were placed immediately after extractions, each equipped with a MED healing abutment to enhance bone metabolism and accelerate osseointegration, addressing the impaired healing potential typically associated with diabetic conditions.


Despite the compromised systemic condition and low bone density, the healing process was remarkably successful. Within less than three months, complete osseointegration was achieved across all seven implants, enabling delivery of the final prosthetic restoration. The use of MED healing abutments significantly improved local bone response, stabilized the peri-implant tissues, and facilitated rapid and predictable rehabilitation in a high-risk diabetic patient with D4 bone quality.
A 50-year-old female patient diagnosed with advanced mandibular cancer and undergoing ongoing biological therapy presented with severe alveolar bone resorption and a fully edentulous lower jaw. Following extractions, four implants were immediately placed using a digitally guided approach to optimize angulation and bone contact. Each implant was equipped with a MED healing abutment, designed to stimulate bone metabolism and enhance osseointegration despite the patient’s compromised systemic condition.
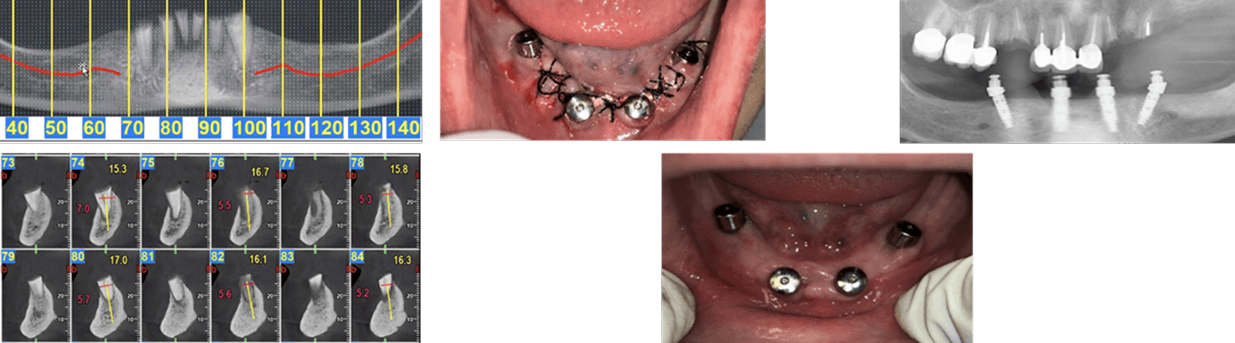
Within 46 days, radiographic and clinical evaluations showed complete osseointegration and excellent soft tissue response, with no signs of inflammation or bone loss. A fixed prosthesis was successfully delivered one week later, providing stable occlusion and high esthetic quality. This case illustrates how MED healing abutments can support rapid bone regeneration and soft tissue stabilization even in medically complex oncology patients with low bone density, enabling early loading and predictable full-arch rehabilitation.
A patient presented with inflammatory environment and advanced crestal bone loss approximately five years after initial implantation. Clinical and radiographic evaluation revealed significant vertical bone resorption and signs of chronic inflammation around the affected implant. A non-surgical regenerative protocol was implemented, involving removal of the existing crown, thorough deep curettage and debridement of the infected tissue, and the placement of a MED healing abutment to promote localized bone regeneration and anti-inflammatory activity through pulsed electromagnetic stimulation.


Radiographic follow-up demonstrated a clear and progressive improvement in bone density and height.
This long-term outcome highlights the regenerative and stabilizing potential of the MED healing abutment as an adjunctive therapy in managing inflammatory environment, even in chronic cases where conventional non-surgical methods typically show limited success. The treatment achieved full functional and esthetic rehabilitation with long-term peri-implant health and radiographically stable bone architecture.
A 55-year-old healthy patient presented with inflammatory environment approximately seven years after successful implant placement. Radiographic evaluation revealed significant vertical bone loss around the implant, indicating advanced peri-implant bone resorption. A non-surgical regenerative protocol was initiated, consisting of removal of the prosthetic crown, deep mechanical debridement and curettage of the infected site, followed by the application of a MED healing abutment to stimulate local bone regeneration and reduce inflammation.


After only one month, radiographs demonstrated clear evidence of vertical bone regeneration around the affected implant, with visible bone fill in previously resorbed areas. The peri-implant tissue exhibited healthy tone and stability, with no bleeding or signs of inflammation. The regeneration process successfully preserved the implant, avoiding the need for complex surgical intervention or implant replacement. This case highlights the role of MED technology as an effective adjunctive treatment in the non-surgical management of inflammatory environment, promoting rapid bone healing and long-term implant stabilit
A 70-year-old healthy patient presented with inflammatory environment and advanced vertical bone loss around two adjacent implants supporting a fixed bridge. The treatment protocol included removal of the prosthetic bridge, thorough non-surgical debridement and deep curettage of the affected sites, followed by the application of MED healing abutments to promote bone regeneration and reduce inflammation through localized electromagnetic stimulation.
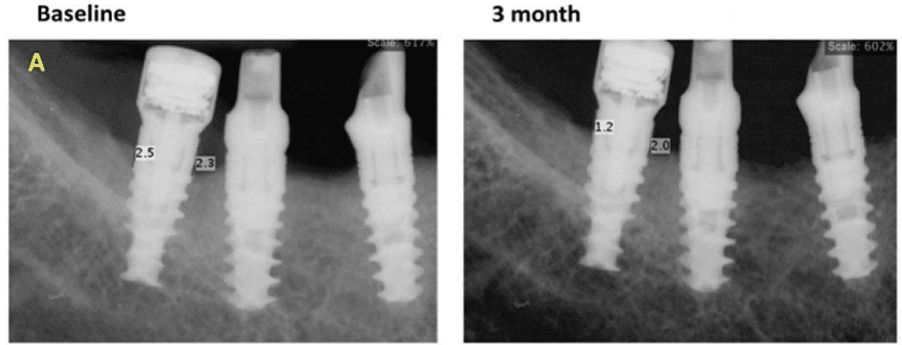

Within three months, radiographic evaluation revealed substantial vertical bone regeneration, effectively restoring nearly the entire height of the previously resorbed bone. Bone levels improved from 2.5 mm and 2.3 mm of loss at baseline to 1.2 mm and 2.0 mm of residual pockets, representing approximately 100% recovery of the lost bone height. The regenerated bone exhibited dense, well-integrated structure, and the peri-implant tissue remained healthy with no recurrent inflammation.
Author: Magdent Editorial Team
Published on: 07 March, 2026
Author: Benny Barak
Published on: 10 October, 2025
Author: Benny Barak
Published on: 08 October, 2025
Subscribe to our newsletter to stay up to date on Magdent’s latest developments and news.
Let us know how we can support. We're here to provide support and answers to your clinical or technical questions.