Author:: Magdent Editorial Team
Published on:: 07 March, 2026
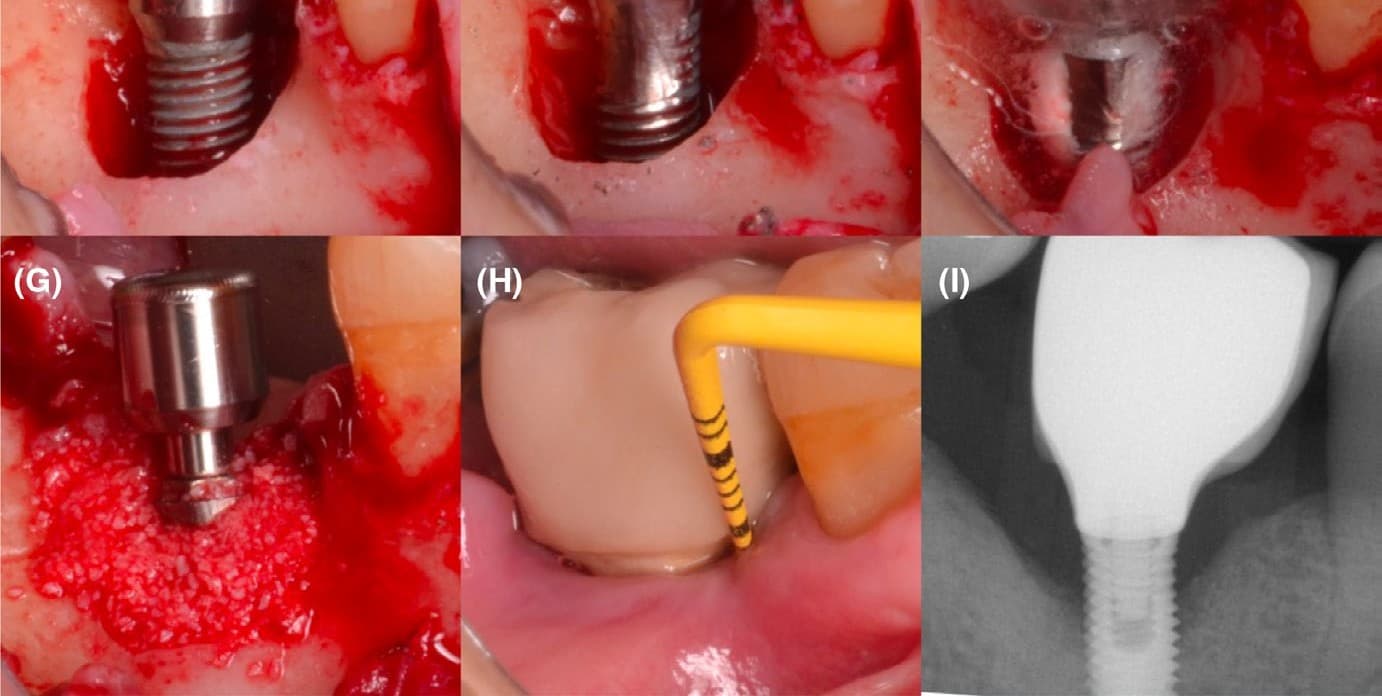
Peri-implantitis remains one of the most frustrating clinical challenges in implant dentistry. Despite decades of mechanical debridement, antiseptics, and locally delivered antimicrobials, long-term predictability remains variable, particularly in complex defect configurations and inflammatory environments.
As highlighted in Dr. Alberto Monje’s review, Emerging locally delivered antimicrobial and immunomodulatory approaches for the prevention/treatment of peri-implant diseases published in Periodontology 2000, peri-implant diseases are not merely infectious complications. They are dysbiosis-mediated inflammatory disorders occurring in susceptible hosts. This distinction changes how we think about treatment.
The traditional therapeutic focus has centered primarily on:
While these approaches can provide clinical benefits, the review clearly emphasizes that the current body of evidence remains heterogeneous and, in many cases, insufficient to establish definitive long-term recommendations for daily practice.
Importantly, the review highlights that implant sites demonstrate early bacterial colonization and strong susceptibility to inflammatory responses. The complexity of defect morphology further complicates prognosis. When managing peri-implant bone defects, clinicians must meticulously evaluate:
These parameters significantly influence regenerative potential, particularly in reconstructive interventions.
For decades, treatment strategies have primarily aimed to eliminate bacteria:
While these approaches target the microbial component, the review emphasizes that inflammation resolution is not always achieved by bacterial reduction alone. Chronic peri-implant inflammation may persist if host response mechanisms fail to return to homeostasis.
This has led to increasing academic interest in adjunctive strategies that do not replace surgery, but aim to support biological healing alongside it.
One of the key insights of the review is that inflammation resolution is not simply achieved by bacterial elimination. Chronic inflammatory conditions may persist due to failure of immune resolution mechanisms.
This understanding opens the door to biologically supportive strategies that go beyond antimicrobial suppression.
Emerging technologies are now being explored that aim to support:
Among the experimental adjunctive modalities currently under academic investigation are advanced surface modifications, laser-assisted decontamination strategies, locally delivered immunomodulatory agents, and bioactive technologies designed to influence cellular signaling pathways.
These approaches share a common objective: not to replace established surgical or mechanical protocols, but to support biological resolution and tissue regeneration in complex inflammatory environments.
Pulsed Electromagnetic Field (PEMF) technology is one of the modalities being explored in this context. Preclinical and clinical research has investigated its potential to influence osteogenesis, angiogenesis, and inflammatory signaling at the cellular level.
Published studies suggest that PEMF may support:
These mechanisms are considered biologically supportive and are being evaluated as adjunctive measures alongside conventional implant therapy. For peer-reviewed studies and publications, see Magdent’s Clinical Research page.
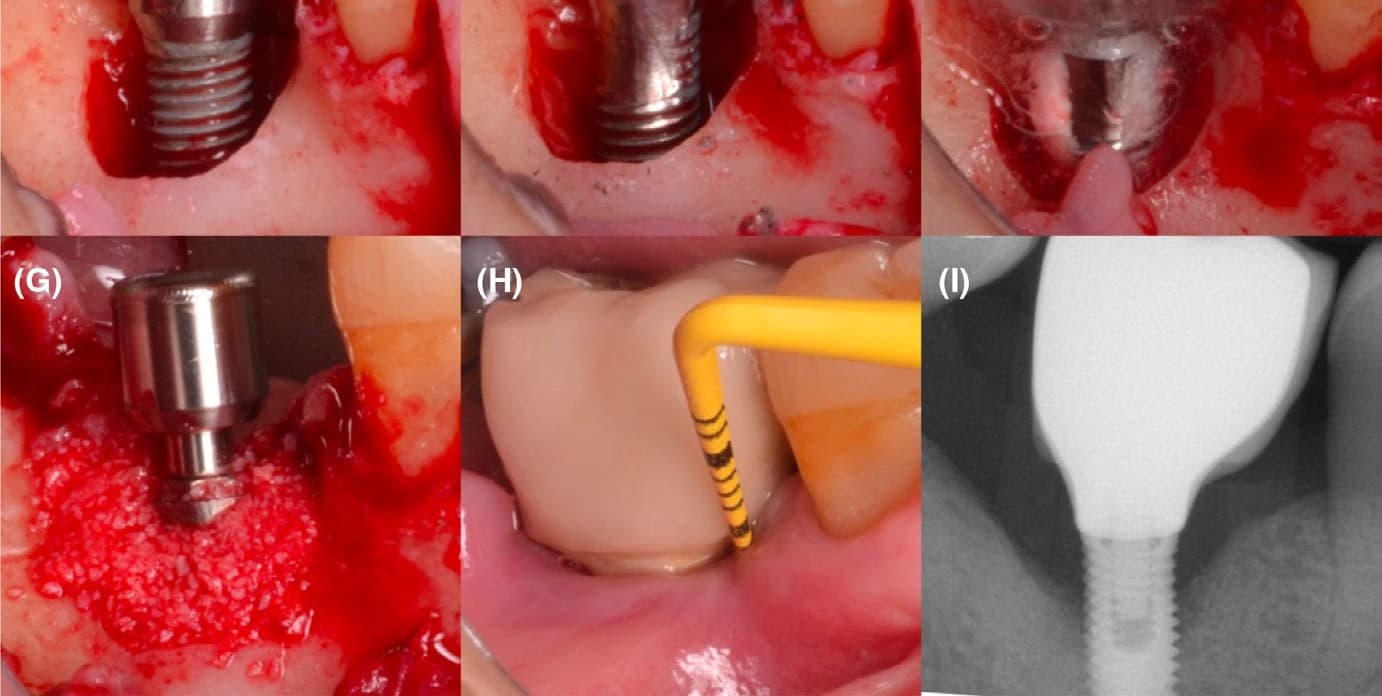
Figure: “Beyond Antimicrobials” visual from the referenced scientific publication context. Source: original publication asset provided (Beyond-Antimicrobials.jpeg).
Within academic and clinical research environments, leading clinicians are actively evaluating PEMF as an adjunctive measure in complex implant cases, including inflammatory peri-implant conditions.
Magdent is honored to collaborate with internationally recognized researchers such as Dr. Alberto Monje, whose scientific contributions continue to shape modern implantology. Learn more about Magdent’s scientific leadership and mission on the About Us page.
Magdent’s Miniaturized Electromagnetic Device (MED) is designed to support osseointegration and biological healing around dental implants. It is not indicated for the treatment or prevention of peri-implantitis and is not a replacement for established surgical, mechanical, or antimicrobial protocols.
PEMF is currently being explored in academic settings as an adjunctive modality that may support tissue response in inflammatory environments when used alongside conventional therapy. Any incorporation into clinical protocols should be considered complementary to, and not a substitute for, evidence-based surgical management. For related context, visit Magdent’s Peri-implantitis page.
The review in Periodontology 2000 underscores a broader evolution in implant therapy: a movement from purely mechanical and antimicrobial strategies toward biologically guided healing approaches.
As our understanding of host-biofilm interactions deepens, the integration of regenerative signaling support may become an increasingly important adjunct in complex clinical scenarios.
The future of implant dentistry may not rely solely on stronger chemicals or more aggressive decontamination, but on intelligent modulation of the biological environment to support predictable healing.
Dr. Alberto Monje, DDS, MS, PhD, is a globally recognized expert in peri-implant diseases and regenerative periodontology. With more than 200 peer-reviewed publications and academic appointments in leading international institutions, his work has significantly contributed to advancing understanding of inflammatory peri-implant conditions and therapeutic strategies.
This article is a thought-leadership summary based on the review:
Emerging locally delivered antimicrobial and immunomodulatory approaches for the prevention/treatment of peri-implant diseases, A. Monje, Periodontology 2000, 2025.
The referenced publication discusses prevention and treatment strategies for peri-implant diseases within a scientific and academic context.
Magdent’s Miniaturized Electromagnetic Device is designed to support osseointegration and biological healing around dental implants. It is not indicated for the treatment or prevention of peri-implantitis or peri-implant mucositis and is not intended to replace established surgical, mechanical, or antimicrobial protocols.
Descriptions of emerging technologies in this article reflect academic research discussions and do not constitute approved clinical indications. Any clinical use remains the responsibility of the treating clinician.
Subscribe to our newsletter to stay up to date on Magdent’s latest developments and news.
Let us know how we can support. We're here to provide support and answers to your clinical or technical questions.